The TAP block is a regional anesthesia technique used for postoperative analgesia in abdominal surgeries. It involves injecting local anesthetic in the neurofascial plane between the internal oblique and transversus abdominis muscles [1,2]. This block targets the abdominal wall nerves, specifically the T7-L1 spinal nerves, to reduce pain [3]. TAP block has been compared to other analgesic techniques and has shown to provide better early postoperative analgesia with almost no complications [4]. It has been found to be equally effective in managing pain after abdominal surgery in pediatric patients [5]. TAP block has also been used successfully in elderly patients undergoing lumboperitoneal shunt surgery, providing quick relief from postoperative abdominal pain. Overall, TAP block is a valuable technique for postoperative pain control in lower abdominal surgeries, offering analgesic benefits and reducing the need for opioids. Local anesthetic systemic toxicity (LAST) is a potential complication of regional blocks, occurring when too high a dose of local anesthetic is accidentally injected intravascularly. It can lead to neurological and cardiovascular manifestations, and early recognition and intervention are crucial for patient management [6]. Patients at extremes of age or with organ dysfunction are at higher risk for LAST [7]. Techniques such as using ultrasound guidance, aspirating prior to injection, and utilizing the minimal local anesthetic dose needed can help reduce the risk of LAST [8]. Intravenous lipid emulsion 20% is the mainstay of treatment for LAST [9]. Complications of local anesthetic systemic toxicity include local anesthetic systemic toxicity, which can occur with peripheral blocks of the hypogastric plexus under fluoroscopy [10]. Local anesthetic systemic toxicity can give rise to neurological symptoms that may or may not be associated with hemodynamic instability. Accidental puncture or trauma to abdominal wall nerves during a transversus abdominis plane (TAP) block can potentially cause temporary or permanent numbness or pain [11].
The Literature Review
This literature review aims to explore and analyze the disadvantages associated with the TAP block procedure and its impact on patient outcomes. By examining existing research studies and clinical trials, we seek to provide a comprehensive overview of the limitations, complications, and challenges related to the TAP block technique.
Potential Complications
One potential disadvantage of the transversus abdominis plane (TAP) block is the risk of nerve injury. Accidental puncture or trauma to abdominal wall nerves during the TAP block procedure can lead to temporary or permanent numbness and pain in the affected areas. Proper ultrasound guidance during needle and catheter placement can help minimize this risk [12,13]. However, nerve injury remains a potential complication of TAP blocks that patients should be aware of. Careful identification of abdominal wall anatomy and avoiding direct nerve contact as much as possible can help reduce the risk of this disadvantageous outcome [14]. Other rare complication is inadvertent puncture of underlying organs, such as the liver or intestines, during needle insertion for the block [15]. This can lead to issues like bleeding, infection, or organ injury. Another potential complication is catheter dislodgement when using a catheter infusion technique for continuous pain relief [16]. If the catheter becomes displaced, it can interrupt the intended pain relief from the local anesthetic infusion. To minimize these risks, practitioners should take precautions such as proper patient selection, use of ultrasound guidance, careful needle and catheter placement, and secure fixation [17]. It is important for patients to be aware of these potential complications to provide informed consent for the procedure [18].
Limitations in Analgesic Effect
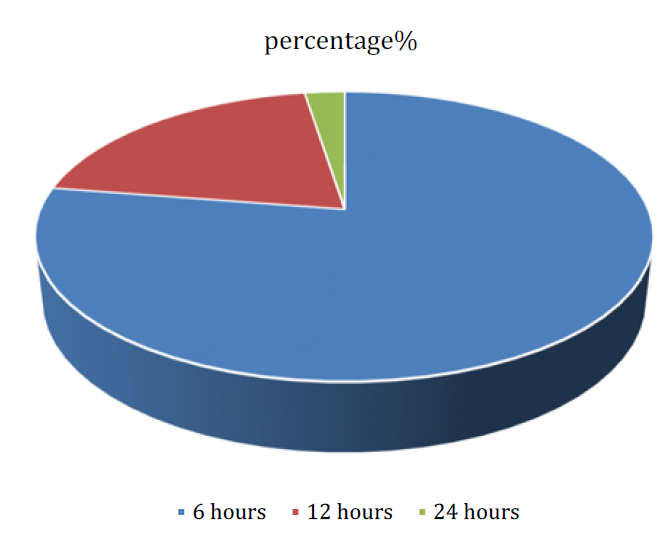
The TAP block has a shorter duration of analgesia compared to epidural analgesia. Studies have shown that the analgesic effect of a TAP block lasts for an average of 6-12 hours, while epidural analgesia can provide pain relief for 24 hours or longer [19,20]. The inconsistent spread of local anesthetic during a TAP block is a limitation due to anatomical variability, making it difficult to reliably block all the nerves innervating the anterior abdominal wall. As a result, some areas may still experience postoperative pain despite the block [21]. The TAP block primarily targets the nerves of the anterior abdominal wall and may not provide deep visceral analgesia like epidural analgesia. It does not penetrate deeply enough to block nerves supplying the internal organs and posterior abdominal wall [22,23,24].
Patient Factors
The transversus abdominis plane (TAP) block is a regional anesthesia technique that can provide effective pain relief after abdominal surgery. However, in obese patients, needle placement for TAP block can be more difficult due to excessive subcutaneous fat. This can lead to inadequate needle positioning, failed regional analgesia, and possible related risks [25]. TAP block with coagulopathy can increase the risk of bleeding with needle insertion, which is a concern for patients on antithrombotic drugs. Bleeding complications after peripheral nerve blocks (PNBs) in patients treated with antithrombotic agents are rare but can result in significant morbidity and may require interventions [26]. The risks of bleeding after PNBs depend on various factors such as block depth, associated comorbidities, anticoagulation status, and technical factors [27]. In the context of image-guided core-needle breast and axillary biopsy (CNB), bleeding is a common complication, and the management of antithrombotic therapy in these patients is still not standardized [28]. A joint guideline from the European Society of Anaesthesiology and Intensive Care and the European Society of Regional Anaesthesia recommends specific time intervals for the administration of antithrombotic drugs before and after nerve blocks to reduce the risk of hematoma formation [29]. The efficacy of TAP block in morbidly obese patients undergoing laparoscopic bariatric surgery is still under discussion, considering the challenges in ultrasound visualization due to excessive subcutaneous fat [30]. In patients on dual antiplatelet therapy or direct-acting oral anticoagulants undergoing high-bleeding risk cardiovascular surgery, bleeding rates range from 18% to 41%, and various potential solutions to mitigate bleeding complications are being explored. TAP block is a method of providing postoperative analgesia after abdominal surgeries, including caesarean section (CS) [31,32]. It has been shown to be effective in reducing postoperative pain and the need for analgesics [33]. However, in pregnant patients, there are concerns about the effects of local anesthetic on the fetus, and the use of TAP block during obstetrical paracervical block anesthesia is contraindicated due to the risk of fetal bradycardia and death [34]. Therefore, it is important to weigh the benefits and risks of TAP block in these patient populations and to consider alternative pain management strategies when necessary [35].
Skill and Training Required
Training programs, workshops, and hands-on practice are essential for clinicians to acquire the necessary skills and knowledge to perform TAP blocks effectively and safely [36]. Clinicians must develop proficiency in using ultrasound equipment, interpreting ultrasound images, and accurately identifying the relevant anatomical structures [37]. Inexperienced users can teach themselves to gain significant procedural skills, but participating in training courses or practicing with experts can enhance the outcomes [38]. Learning to perform TAP blocks with ultrasound guidance has a learning curve, and clinicians need to understand the indications, clinical pearls, and pitfalls of each procedure to avoid potential complications [39]. Residents demonstrated improvement in ultrasound-guided procedural skills and reported increased comfort performing these procedures after training on an agar model [40]. Ultrasound increases the first-attempt success rate for vascular access, and competency on ultrasound-guided peripheral intravenous cannulation can be achieved after following a brief training in a fixed curriculum. In the absence of ultrasound guidance, accurate needle placement during TAP blocks can be challenging, leading to suboptimal pain relief or block failure. Without visualizing the target nerves and adjacent structures, clinicians may struggle to locate the neurovascular plane accurately, resulting in inadvertent needle placement into unintended tissues or structures [41]. Ultrasound-guided nerve blocks provide real-time visualization of needle placement, allowing for accurate drug injection around the nerve or into the nerve in some cases [42].
This technique is considered safer and more accurate than the conventional landmark-based technique, particularly for less experienced clinicians [43]. Ultrasound guidance improves the success rate of nerve blocks by improving block operating efficiency, decreasing placement complications, and reducing patient discomfort [44]. To mitigate the risks associated with performing TAP blocks without ultrasound guidance, alternative techniques such as landmark-based approaches or nerve stimulation can be employed. These techniques rely on anatomical landmarks or nerve stimulation to guide needle placement. However, they are generally considered less reliable and have a higher risk of incomplete or inaccurate blocks [45,46,47]. Ultrasound guidance technique, on the other hand, allows for real-time visualization of needle placement and accurate drug injection around the nerve, resulting in improved success rates and safety [48,49]. Ultrasound-guided nerve blocks provide direct visualization of the target nerve and deposition of local anesthetic, improving block operating efficiency while decreasing placement complications and patient discomfort. Therefore, ultrasound guidance is considered the gold standard for regional anesthesia, particularly for lower extremity blocks. Ultrasound guidance is recommended for performing transversus abdominis plane (TAP) blocks as it reduces the risk of incomplete or inaccurate needle placement, improvingthe effectiveness and safety of the block [50,51]. However, clinicians need to undergo training and gain proficiency in ultrasound imaging and needle guidance to perform TAP blocks accurately [52]. Without ultrasound, there is an increased risk of complications and compromised block efficacy [53]. Clinicians should consider the benefits and limitations of different techniques for TAP blocks and choose the approach that aligns with their skills and resources [54].