After obtaining approval from the Institutional ethics committee, CTRI registration number CRTI/2020/10/028306 and written informed consent of the patients, the proposed study was carried out in adult female patients of age groups 18-60 years, visiting the pain clinic for chronic pelvic pain, who had already taken medications for 2 weeks but inadequate benefit was reported by medications and physiotherapy trial.
Source of Data
This study was conducted on patients with chronic pelvic pain at IGMC and associated hospital KNSH for M and Ch Shimla with the approval of research and Ethics Committee.
Study Design
This study was randomized, single blinded prospective and controlled study.
Inclusion Criteria
Patient giving consent to participate in the study
Female patients with chronic pelvic pain after ruling out any obstetrics and gyanecological cause through specialist opinion and USG or negative diagnostic laproscopy
Patients above the age of 18 years and below 60 years
Patients who have had atleast two weeks trial of medications without significant effect
Patient with normal anatomy for ganglion impar block
Exclusion Criteria
Patient refusal
Patients with uncontrolled systemic diseases
Patients with infection or injury at the injection site
Patients with coccygectomy
Allergy to iodine contrast medium
Hypersensitivity
Patient with bleeding disorders and the patients on anticoagulants
A total of 30 patients from pain clinic who were suffering from chronic pelvic pain were included after obtaining written consent.
Sample Size Calculation
The sample size was calculated to be of 15 subjects for each group; this was calculated on the basis of a similar study in chronic pelvic pain patients where the minimum number of patients required were found to be 31, with a power of at least 80% and α of 0.05. Anticipating loss of subjects during the study, we enrolled 30 patients in our study, 15 in each group.
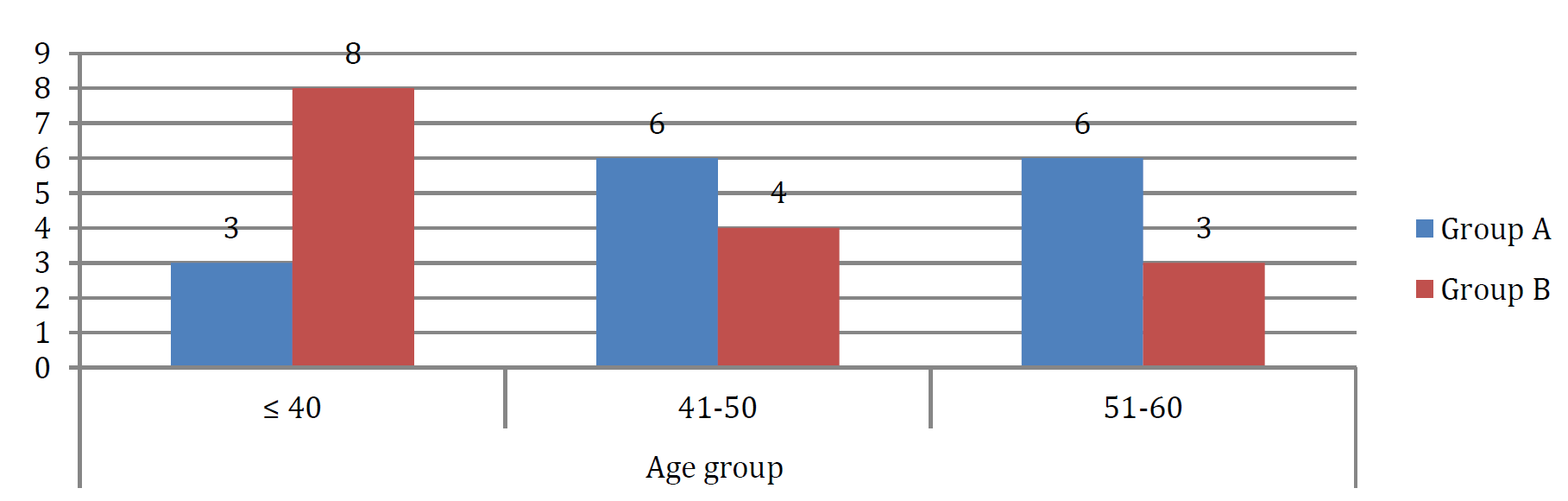
The patients were divided into 2 groups of 15 patients each using computer generated random numbers.
The study was randomized, single blinded prospective and controlled study with follow up done weekly for three weeks either by routine checkup in the pain clinic or through a phone call. They underwent radiofrequency ablation of Ganglion Impar by trans-sacro-coccygeal technique using C-arm guidance.
Patients were made familiar with American Chronic Pain Association Quality of Life Scale. The ganglion impar block was administered in all these patients under all aseptic precautions using C-arm guidance to mark and identify bony landmarks.
Methodology
All patients underwent a routine preanaesthetic checkup. During this, thorough history, general examination, routine investigations of the patients i.e. FBS/RBS, bleeding time (BT), clotting time (CT) of the patient was carried out. Quality of life was assessed using American Chronic Pain Association Quality of Life scale.
After confirmation of inclusion criteria of the patient by the anesthesiologist the procedure was undertaken. Written informed consent was taken from the patient prior to the procedure explaining the various risks and benefits of the procedure. A 20-gauge venous access was secured and basic monitors such as noninvasive blood pressure, and saturation (SpO2) probe will be connected.
The procedure was carried out with the patient in prone position with pillow under the abdomen to allow flexion of the lumbosacral spine and the lower extrimities rotated internally.
The procedure was performed using C-arm to identify and mark the essential bony landmarks. Under strict aseptic precautions the saccrococcygeal and gluteal regions were cleaned with savlon and painted with povidone iodine 10%. The area was drapped with sterile towels, and the access region was left open. A skin wheal was raised with 1% lidocaine using 25-gauge needle after the identification of the disc in lateral projection. A true lateral image was obtained by superimposing the two greater sciatic notches.
22G, 5 cm long with 5mm active tip radiofrequency needle was then introduced from the marked site to pierce the saccrococcygeal joint and position was confirmed after injecting non-ionic dye and needle placement was confirmed by induction of reverse comma sign/ “crescent” sign in lateral fluroscopic views. A diagnostic block was performed using 1% lidocaine 10ml.
After 5 min, patient was ressessed and if the patient considers pain relief of atleast 2-point reduction in VAS scores, the patients were considered candidates for radiofrequency ablation of Ganglion Impar.
Before radiofrequency ablation was performed, tissue impedence check and motor and sensory tests were done. These comprised tissue impedence <600 Ohm, sensory response <50 Hz and motor response < 2 Hz at stimulation intensity between 0.4 – 0.8 volts. Patients with no significant decrease in VAS score were excluded from this study.
Thereafter radiofrequency ablation was done depending upon the group:
Group A: Thermal radiofrequency ablation, was done using radiofrequency thermocouple electrode (Cosman Medical Co Inc.) connected to Cosman radiofrequency generator using following parameters: tissue impedance <600 Ohm, sensory response <50 Hz, and a motor response <2 Hz at a stimulation intensity between 0.4–0.8 volts (V) with 3 cycles each 90 seconds apart and temperature ranging from 60 -80°C
Group B: Pulsed radiofrequency ablation, was done using radiofrequency thermocouple electrode using the following parameters: voltage output 45 V, 2 Hz frequency, 20 ms pulses in a one-second cycle, 120 second duration per cycle, impedance range between 150 and 500 Ohms with 3 cycles and a 42°C plateau temperature Inj bupivacaine 5ml and inj dexamethasone 2 mg was injected the end of procedure to overcome ablation induced pain and neuritis. Follow up was done after the procedure using American Chronic Pain Association Quality of Life Scale
Patients were kept in the recovery room for 2 hours and then sent home with the attendents on the day of the procedure with routine single dose antibiotic prophylaxis, NSAIDS in the form of Tablet Diclofenac 100mg SR for 3 days. Patients were advised to abstain from heavy workload after the procedure. Patient who complained of increase in VAS in between the follow up period were given tablet Pregablin 75 mg H.S. at night as rescue drug. Complains / side effects like parasthesias and numbness were noted.
Follow-up after 24 hours,1 week, 2 weeks and 3 weeks was done either in OPD or telephonically and Quality of Life score were noted.
Failure cases: Patients who did not achieve a successful block, that is patients in whom there is no decrease in VAS by 2 points after 24 hours of block were dropped from further study; but the number was noted as failure cases and other form of treatment was given.
American Chronic Pain Association Quality of Life Scale
0 (Non-Functioning)- Stay in bed all day. Feel hopeless and helpless about life
1 Stay in bed atleast half the day. Have no contact with outside world
2 Get out of bed but don't get dressed. Stay in home all day
3- Get dressed in the morning. Minimal activities at home. Contact with friends via phone, email
4 Do simple chores around the house. Minimal activities outside of home two days a week
5 Struggle but fulfil daily home responsibilities. No outside activity. Not able to work/ volunteer
6 Work/Volunteer limited hours. Take part in limited social activities on weekends
7 Work/ Volunteer for a few hours daily. Can be active atleast 5 hours a day. Can make plans to do simple activities on weekends
8 Work/ Volunteer for atleast 6 hours daily. Have energy to make plans for one evening social activity during the week. Active on weekends
9 Work/ Volunteer/ be active 8 hours daily. Take part in family life. Outside social activities limited
10 (Normal Quality of Life)- Go to work/ volunteer each day. Normal daily activities each day. Have a social life outside of work
Data Analysis
All the data collected from the patient’s records was transferred into MS Excel sheet for further processing and analysis. Data was further analyzed using standard statistical software. In order to compare results between two study groups, appropriate parametric or non-parametric test of statistical significance was used. Probability value (p-value) less than 0.05 was considered statistically significant.