Source of Data
Patients suffering from Sinonasal Polyposis attending routine ENT OPD in Dr. RPGMC Tanda.
Methods of Collection of Data
Study Area: Department of ENT, Head and Neck Surgery in Dr. RPGMC Tanda.
Study Population
30 patients of Chronic Rhinosinusitis with Nasal Polyposis.
Study Design
Hospital based cross sectional study.
Study Period
One Year, i.e. from June 2018 to June 2019.
Inclusion Criteria
Study population included adult population (>18 years) suffering from CRSwNP who were not taking any treatment at least for the last 1-2 weeks, diagnosis being made on basis of history and clinical examination.
Clinically patient having following symptom was included:
Sneezing
Itching in nose, eyes, ears and palate
Nasal discharge
Nasal obstruction
Loss of smell
Facial Pain or pressure
Headache
Nasal polyposis
Patients not on medication for the past 2 week.
All patients willing to give consent.
Exclusion Criteria
Patients didn’t willing to give consent.
Patients aged <18 years.
Patients suffering from diseases like:
DNS
Adenoid hypertrophy
History of Sinonasal surgeries (for recurrent nasal polyp)
Patients with cystic fibrosis
Patients suffering from fungal sinusitis
Patients with immunotherapy
Pregnancy
Nasal neoplasm
Patients who have used nasal, inhaled or systemic steroids within 2 months
Chronic bronchitis
Bronchial asthma
Methodology and Type of Data Collected
Present study was conducted in the Department of ENT in Dr RPGMC Tanda, after obtaining clearance and approval from the institutional ethical committee; patients fulfilling the inclusion/exclusion criteria were included in the study after obtaining informed consent. Blood drawn from median cubital vein under all aseptic conditions in labelled EDTA vial for each patient was sent to centralized laboratory of the Institute for complete haemogram test and thus peripheral blood eosinophil count was obtained in all patients prior to surgery.
Blood eosinophil count ≥ 6 % of differential leucocyte count in CRSwNP patient is taken as Eosinophilic CRSwNP while values ≥ 6% are considered as Non eosinophilic CRSwNP.
Following endoscopic sinus surgery, the biopsy of the polyp was sent for histopathological study in the Department of Pathology Dr. RPGMC Tanda. Samples were fixed with formaldehyde solution and later with haematoxylin and eosin staining. Slides were examined for tissue eosinophil count. Tissue eosinophil count was graded as 0, 1+ and 2+ where 0 is no eosinophils while 1+ is occasional or less than 10 eosinophils and 2+ being more than 10 eosinophils /HPF in the sample slide.
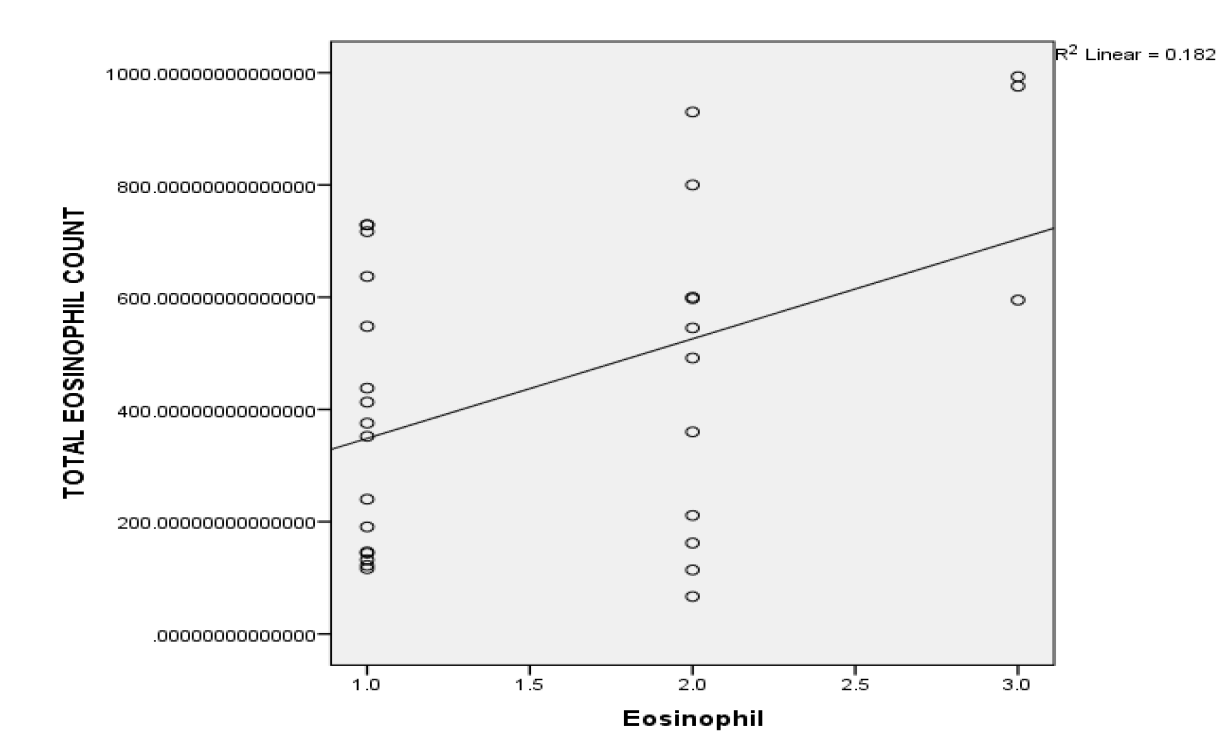
Eosinophilic CRSwNP was defined when tissue eosinophil count was >10/HPF or tissue eosinophil count grade 2+. Both the counts (eosinophilic blood count and histopathological eosinophil count) were compared to know the relation and significance of eosinophil count in sinonasal polyposis.
Statistical Analysis
The data entry and analysis was done in Microsoft Office Excel 2007 and Epi Info software. Descriptive analysis was done using frequency, percentages and Mean (+/-S.D.). Association between Absolute Eosinophil count and histopathological eosinophil count between non eosinophilic chronic rhino sinusitis (NECRSwNP) and in eosinophilic chronic rhinosinusitis (ECRSwNP) groups was determined by applying student ‘t’ test. p value <0.05 was taken as statistically significant.